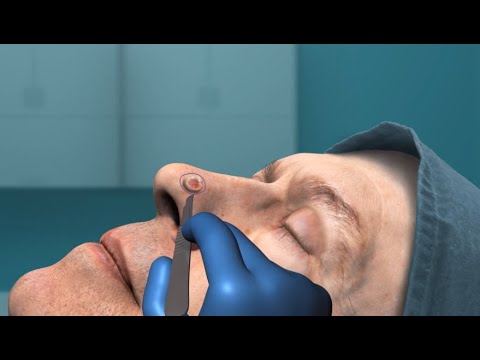
MOHS SURGERY

Schedule your Mohs surgery consultation today.
MORE ABOUT MOHS SURGERY
OUR MOHS SURGEONS

PATRICK SNIEZEK
Patrick Sniezek, MD, is a Mohs Surgeon and the head physician for the Mohs Surgery and Skin Cancer Center at CSDERM, Colorado Springs, CO.

KENDRA TAN
Kendra Tan, MD, is a Mohs Surgeon and dermatologist for the Mohs Surgery and Skin Cancer Center at CSDERM, Colorado Springs, CO.
OUR LOCATIONS
COLORADO SPRINGS CENTRAL
170 Parkside Dr
Colorado Springs, CO 80910
LOCATION INFO & MAP
(719) 471-1763
Dial extension 126 for Mohs Surgery
COLORADO SPRINGS NORTH
2060 Briargate Pkwy, Ste 150
Colorado Springs, CO 80920
LOCATION INFO & MAP
(719) 471-1763
Dial extension 426 for Mohs Surgery
THE MOHS SURGERY PROCESS
About our Mohs surgery center
What does a Mohs surgeon do?
Is Mohs surgery better?
Benefits of Mohs surgery
What happens during the procedure?
What are the risks?
How do I prepare for the surgery?
What happens on the day of surgery?
Medications to avoid before surgery
Unless prescribed by your doctor, do not take aspirin, even a baby aspirin, or products containing aspirin for ten days before surgery. Non-steroidal anti-inflammatory products like ibuprofen and naproxen should be stopped five days before surgery, as should any vitamin supplements containing vitamin E, ginger, gingko, and garlic. Tylenol can be taken at any time before surgery. If you take warfarin (Coumadin) or Plavix, you can continue your regular dosing.
Alcoholic beverages should be avoided 48 hours before surgery, as they can promote bleeding.
What can I expect after the surgery?
Patients may experience temporary swelling around the surgical site, particularly if it is performed near the eyes. Though rare, infection may occur and is treated with antibiotics. Temporary itching in the area may also occur. Sometimes, patients experience temporary or permanent numbness around the surgical area. This is caused by cutting small nerve endings during surgery and normally resolves with time. Particularly when large tumors are involved, there may be a temporary or permanent weakness in the surgical area caused by the severing of a muscle nerve. If we feel this may be a problem in your case, we will discuss it with you before surgery. Though it’s rare to experience loss of muscle function after Mohs surgery, it may occur in a few cases.
What kind of follow-up can I expect?
Will my insurance cover the procedure?
HAVE MORE QUESTIONS?
Schedule an appointment to talk one-on-one with a Mohs surgeon today:
(719) 471-1763
Dial extension 126 for Mohs Surgery
The Mohs Micrographic Surgery Procedure Overview